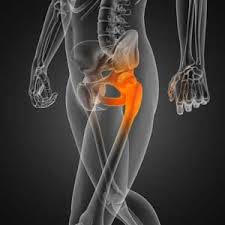
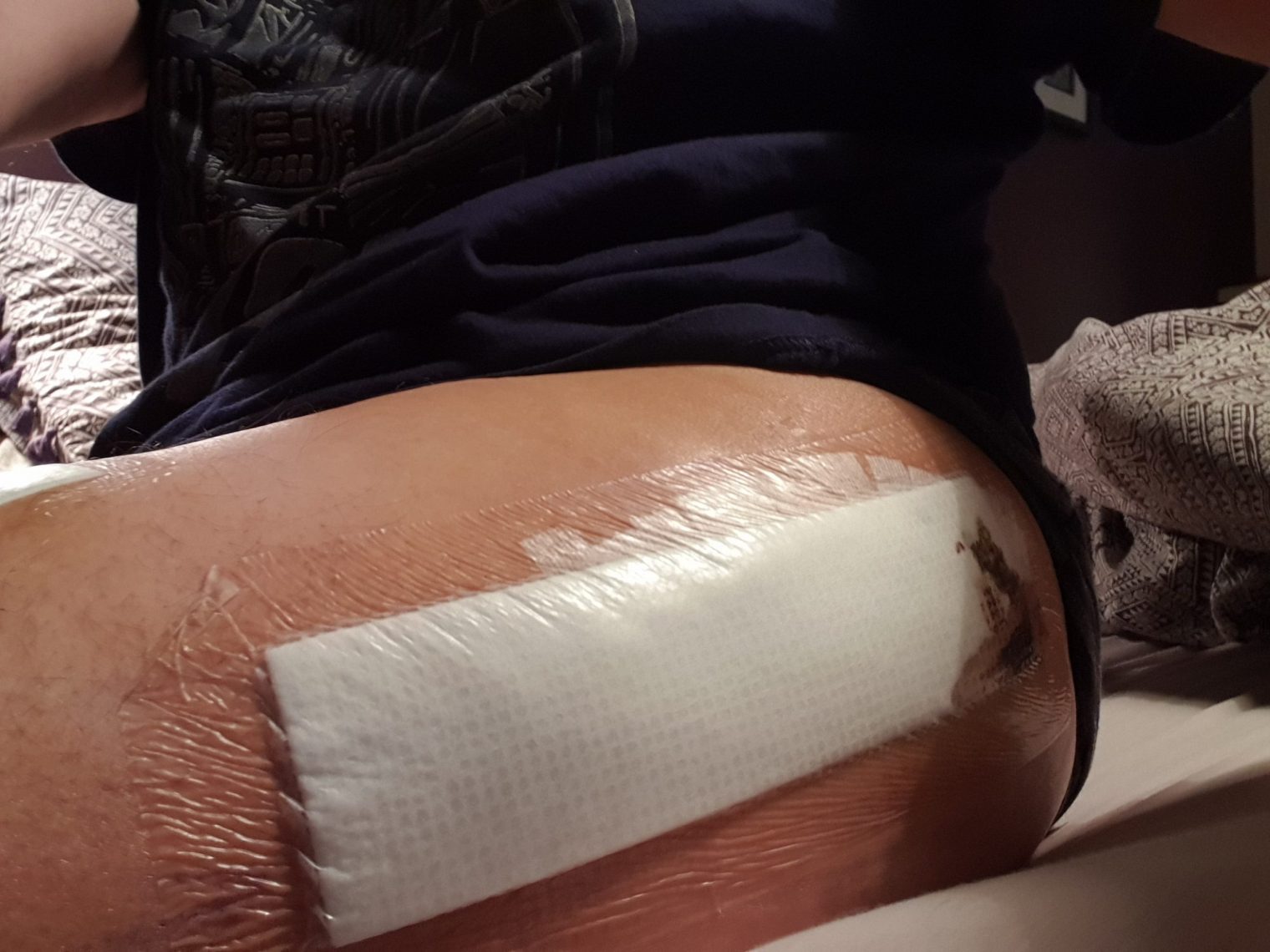
Previously I had been both concerned and excited about by my hip replacement surgery. Part 4 describes the week of the operation, from incision, to infection, to incapacity. It was certainly one to remember.
- Part 1: Midlife arthritis and the underlying problem
- Part 2: Total hip replacement decision
- Part 3: Total hip replacement pre-op assessment
- Part 4: Surgery and hospital recovery: Days 1 to 5
- Part 5: First steps to recovery. Days 6 to 21
- Part 6: Hip recovery limping along. Weeks 3 to 7
- Six months after hip replacement. The review.
- Twelve months after hip replacement. A year in pictures.
Day 1: Surgery day – happy upsides followed by grim downsides
Time ticked by and the big day arrived. At 7am, sipping my last cup of tea and eating my last piece of toast, my main concern was how hungry I might be by 3pm when I was scheduled for the op.
With my entertainment and goody bag packed (books, sweets, chocolates, laptop etc) I headed off to hospital. Part of me was looking forward to some quiet recovery days taking it easy and being waited on.
The pre-operation time passed quickly. On arrival (and possibly the difference between private and NHS) the first thing I had to do do was place my food order for the evening and next day. Starving, I ticked all the boxes and looked forward to my full English breakfast served by nurses, while I watched the TV in comfort. If I had only known then what was to come….
Next I put on the backside exposing gown and disposable pants to create that sexy middle-aged bloke look. The pants had to be stretched, but that was over my backside than for any other reason. I don’t think I had them on for long.
Soon came the stream of doctors and nurses, checking and rechecking my name, d.o.b., vitals, leg, and reassuring me this was a routine operation and quite enjoyable if I relaxed. I signed up to a catheter due to previous post-op problems in that department, and discovered I was having an epidural and sedative rather than general anaesthetic. Oh go on then. How bad could it be?
As I was “so young” (which was to become a recurring theme in discussions) my consultant thought I could be home within 48 hours of the op, so the target was Weds afternoon. I was good to go.
The operation – a chance to discuss life
I walked down to the theatre and climbed on to the bed. Within a couple of minutes I was sedated, and wheeled into theatre chatting happily to the nurses about life.
Separating me from my bottom half was a blue sheet, beyond which the consultant and his team did their stuff. Being awake I could hear some of the conversation. He started off by saying “that’s a schoolboy error” about something. It was a test of the sedative. I laughed without a care.
The next two hours were a bit bizarre. While I chatted away to the anaesthetist, I could feel my leg being pulled, and one point being hammered, and at another other being twisted. However it didn’t hurt and I didn’t care. The anaesthetist even brought the old broken joint out for me inspect. He showed me the problem (holes and general wear). I think this was to make sure I gave them a high feedback score for “value for money” in my patient survey.
I asked to keep the joint, but this was politely declined. Medical waste apparently.
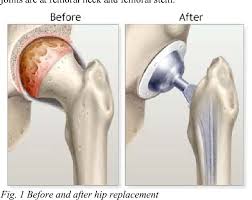
When it was finished the surgeon came round, took off his full-face mask and shook my hand. Because I was so young (again) I had had a cementless joint (there are pros and cons of this), but he felt my bone would naturally grow round it and it could make any second operation easier. It was all very bullish, but things were brewing neither of us knew.
Following a short spell in the recovery room chatting to (or boring) the nurses with how good I felt, I was wheeled back to my room. I wasn’t hungry, but had no real pain, so when the food arrived I manfully worked my way through it. Next I made a few phone calls and sent some texts to tell everyone how successful the hip replacement surgery had been.
My legs started to tingle and move as the epidural wore off. It was great. Life was good.
Crash and burn – a grim way to recover from hip replacement surgery

By ten o’clock it was time for bed and meds. The nurse came in, got me to swallow some tablets and was just walking out the door when I felt a bit sick.
I called her back, and it all started to go wrong. As she hurried over to me with a cardboard hat, I started to vomit, then shake and sweat. All of a sudden I felt very poorly.
Within what seemed like seconds there were loads of people in the room. I remember the doctor asking me how I was feeling, and me telling him I couldn’t see him any more before it all went black.
Apparently my blood pressure dived at the same time my temperature shot up. Some people have a reaction to surgery, which can cause the low blood pressure, but the temperature meant it was more likely an infection,
After that it was a blur. I remember lying on the bed with an oxygen mask on. Joy, my night nurse had to keep removing it so I could be sick. I couldn’t work out that lifting it up was better than pushing it down like a dribble (or vomit) catcher. I remember hearing the doctor phone the consultant and anaesthetist, and discuss me going to a&e for a blood transfusion. I remember them taking blood until the point they couldn’t any more. I was running dry on lots of levels, but attached to plenty of drips and technology to ensure things stabilised.
At one point they also wanted to get an Xray of the hip joint as it was more swollen than expected, but being unable to travel they brought a machine to me. Four strapping 5ft tall nurses had to lift me in my blanket so they could slide the plate under me. Luckily I’m light. Or not. At least when they then wanted a chest x-ray it was a much easier proposition.
The one upside was that when they kept asking for urine samples, all they had to do was turn on the tap from the catheter bag. It was like getting wine from a wine box.
By 4:30am things started to calm down, the shaking stopped and I dozed off.
Some routine surgery that had turned out to be.
Day 2: Hip replaced, but not really aware
The following morning I was a bit confused as despite vomiting, being unable to concentrate, talk or stay awake, I still thought I would be home on the Weds as the consultant had told me.
The breakfast and lunch I had so enthusiastically ordered on the previous day were returned untouched.
My wife who had come in expecting a short visit ended up cancelling work and staying all day as i looked so grey. I don’t think I managed to speak much though. All day, people came in doing more tests to try and work out what had happened but to be honest, I slept through most of it.
The physio did get me to stand up, but decided a shuffle to the door with the zimmerframe would be too much so steered me back to bed.
Gradually though I was starting to feel better. Honestly.
One final trauma, but not really related to the hip replacement surgery
About 10pm they decided to remove the catheter as that was becoming the prime suspect for the infection. Deep breath in, hold, and slowly out.. and ouch…
Now another trauma awaited.
In a previous operation I had struggled to urinate afterwards, letting my bladder swell and making me sweat. When I was handed the bottle late that evening, I placed it between my legs and prayed. Then thought of something else. Then whistled a tune, but nothing was happening down there. Psychological issue? Oh yes, I have plenty of those.
Given I was drinking like a fish and still taking on board litres of fluid from the drip, it wasn’t long before I capitulated and rang the bell. Around 1 am Nurse Joy arrived to help.
Nurse Joy suggested a mobile commode. So canulas were briefly disconnected and I was helped to the wheelchair type device. Before she left the room she pressed the alarm into my hand in case I ran into trouble. At least I had some privacy.
Ahhh, the relief psychologically and physically was fantastic. A drip, then I was away, smiling in triumph. Well, for about the four seconds it took me to realise there was a puddle forming around my stockinged feet. Something wasn’t connected. I had a panic. Should I continue to relieve, or press the alarm for help and the trauma that might bring? I bottled it and rang the bell. Joy, with typical nursing efficiency and a smile told me it wasn’t a problem, despite having to clear up, wash my legs, get me new stockings and mop the floor. She was a star.
Eventually I was back in bed. Given my fluid intake it was probably only an hour before I needed to go again. I decided to man up, break the psychological barrier and just do it. Amazingly it worked. I pressed the buzzer and Joy came in beaming with delight. We shared a happy moment agreeing both the quantity and colour of my urine were great signs of recovery.
After that it was non-stop disruption that night – bottle swap, vitals check, drip alarm to be turned off each time I moved. Me and Joy shared another night of pretty constant contact.
Day 3: Getting back to life – up and about

On Wednesday things began to get back on track. As by now a man of mystery I received high quality care and attention. They couldn’t work out any cause of the infection as all the tests were coming back negative.The prevailing thoughts were that I suffered a bleed in the wound (apparently more common in young, muscular men like me – honestly?!) which may have combined with an infection I brought in or got when the catheter swept bacteria into my body as it was inserted. Just unlucky.
On this day I actually made a solo trip to the bathroom with the zimmerframe, so the bottle trauma started to come to an end. The physio gave me some bed exercises (muscle squeezing, knee bending), and took me on a small trip outside the room, but still with the frame.
As my blood was still low in haemoglobin they didn’t want to push me, and I was exhausted. But now I felt I was on hip recovery rather than operation recovery.
She also got them to change the air mattress for a normal one, which suddenly meant I could hear the TV and getting in and out of bed became much easier.
To be fair it wasn’t all bad. I still had no pain from my hip, which was good going. I was only on Naproxen and Paracetamol (ignoring the blood thinning injections, antibiotics, anti-nausea stuff) as they didn’t want to give me strong painkillers following by funny turn on Monday night.
Day 4: Doing the basics – showering, shoes, shaving and other stuff starting with ‘sh’
Thursday and things were much calmer. I managed breakfast (Special-K – I had given up on the cooked breakfast). Again had the doctor explained I was unique as they couldn’t find a cause (the catheter was still taking a lot of blame). Although my haemoglobin was still too low, given I was so young (“say that again” I asked once more) they decided not to transfuse. They didn’t want the infection risk and thought with iron tablets and a healthy dose of liver or two I should recover in a couple of weeks). A cynic might say cost could have been part of it, but I believe they did have my interests at heart.
The drugs continued to flow, and laxatives were added in to the mix. All a bit shit really. Ho ho.

I was invited to shower. Great until I realised I couldn’t reach the towel, dry myself beneath my knees or get myself dressed. When I asked for help I couldn’t help but think that in a younger life (and in a Carry on Doctor sort of way) I had fantasised about events like this. The truth is, when you’re feeling like shit, frustrated and tired you just appreciate the way the nurses get on with their job and ignore your slightly misshapen middle-aged body.
I sat in the chair for a bit, then got myself to bed and back to the chair. I had a friend call in to see me for half and hour or so, but I’m not sure I was the best company.
The physio had now got me moving on crutches, and I did a corridor shuffle to add to the exercises.
Day 5: Friday I’m in love with. Going home post hip replacement surgery.
Finally they decided I could go home. I completed the “two crutch test” of corridor, slope and stairs so the physio could sign me off as home ready. To be honest I still felt a bit crap and my entertainment bag was untouched.
I also had to pass the self injection test (Fragmin, for blood thinning). My test run was on a stuffed sock. I had to laugh when they asked whether I could find a roll of fat to inject. I had been in training for that question for many years with some devoted cake eating.
My first attempt saw me wipe the site afterwards leaving me a lovely bruise, but although unpleasant it was OK. Hats off to all those people who have to do that every day.
There was one more struggle to get past in going home – getting in and out of the car. Stand sideways with your bum facing the seat, slide across until your bum breaks the gear stick. Swing round slowly, groan, and then relax.
And then I was home. Uncommunicative, tired, and nauseous, I was a joy to be with. But actually I was feeling better, and more positive, looking forward to the day by day improvements to come.
The week that was. Hip replacement surgery complete.
So in summary, for those who may face hip replacement surgery….
- I was unlucky to get an infection – most people don’t. The upside of the infection was my chocolates, biscuits and cake remained untouched.
- Epidural and sedative is to be recommended, it’s much more entertaining than being asleep and you don’t care about what’s going on.
- There isn’t a lot of hip pain from the operation, and any old hip pains disappear immediately.
- You’re up and about surprisingly quickly in terms of the hip replacement recovery timeline, but be careful. It’s easy to reach, twist or stretch too far. They tell you some horror stories to make you more aware, but the chances of things going wrong are slim
- You can’t do it all yourself – drying, dressing and carrying things are pretty impossible to begin with.
- Nurses demand respect. They have to do some really naff things.
Official NHS hip replacement recovery tips can be found here.